This article provides step-by-step instructions on how to file a corrected claim in Elation Billing.Documentation Index
Fetch the complete documentation index at: https://help.elationhealth.com/llms.txt
Use this file to discover all available pages before exploring further.
Overview
What is a Corrected Claim?
A corrected claim is a resubmission of a previously submitted claim with updated information. It includes a correction code and the original claim’s ICN (Internal Control Number) to identify which claim is being corrected.Automatic Corrected Claims
Corrected claims have been partially automated! If the payer has provided an ERA in Elation Billing, simply update and resubmit the claim to file it as Corrected. Our clearinghouse will automatically add the ICN and file the claim as Corrected.
Workflow Instructions
Filing a Corrected Claim Manually
- Navigate to the Claim - Find the claim in your Worklist or locate it in the patient’s chart by clicking Claims.
-
Save the Payer ICN - We suggest adding the ICN to a saved list for reuse:
- Click Corrected Claim Info
- Click Add ICN to List
- Select the Insurance Payer
- Enter the ICN
- Click Save
Finding the ICN
- Go to the Superbill
- Click the Claim History button
- Under the Clearinghouse History section, look for ERA Received
- The ICN will be under the Messages column
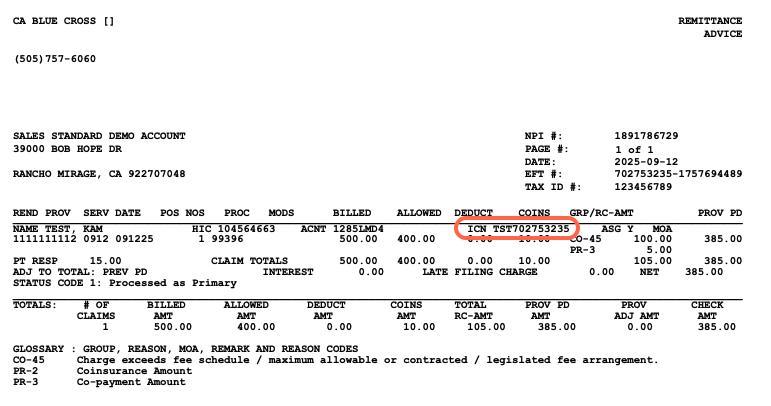
-
Attach the ICN and Correction Code - From the Claim Corrections Screen:
- Select a Correction Code:
- Original Claim (Frequency Code 1)
- Corrected Claim (Frequency Code 7) - All resubmitted claims will have this code and ICN automatically included
- Voided Claim (Frequency Code 8)
- Enter an ICN OR select one from your list by clicking on it
- Click Save
- Select a Correction Code:
The correction code will be attached to the claim for ONE SUBMISSION ONLY. This keeps correction codes from following the claim to subsequent secondary billing.
Once the Corrected Claim has been billed, the Corrected tag will automatically be added.
- Lightning Bill the Claim - Bill the claim to the payer using the usual method.
For information on the disposition of the claim after submitting, contact the payer (typically via their portal).
