Documentation Index
Fetch the complete documentation index at: https://help.elationhealth.com/llms.txt
Use this file to discover all available pages before exploring further.
Overview
What is a claim appeal?
A claim appeal is a formal request to an insurance payer to reconsider a denied or underpaid claim. Appeals include documentation supporting why the claim should be paid or paid at a higher rate.Why are claim appeals important?
Appeals give you the opportunity to recover revenue from claims that were incorrectly denied or underpaid. Including supporting documentation and claim history increases the chances of a successful appeal.Before you begin
- Check the payer’s filing deadline. Most payers require appeals to be submitted within a set window after the original denial (commonly 90, 180, or 365 days). Confirm the deadline on the payer’s EOB or contract before starting.
- Gather supporting documentation. This may include the original claim, EOB/ERA, medical records, chart notes, proof of timely filing, or a letter of medical necessity. This information can be included on the appeal when generating an appeal.
- Review Claim History. Use Claim History to view the full clearinghouse trail for the claim you’re appealing. This information can be included on the appeal when generating an appeal.
Workflow Instructions
Creating a claim appeal
Locate the claim using one of the following workflows:
- The Superbill itself
- Patient record → Claims → Charges
- Billing → Claims Manager
In the window that appears, select whether or not you want the original claim form and then click Appeal → Start. This will open a new window for you to complete the appeal.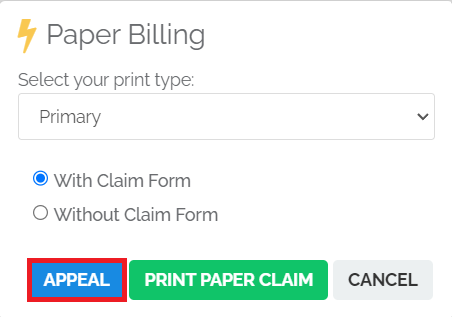

Review the Appear Options:
- Select the type of Appeal Form you want to use
-
Specify whether you want any of the following included with the appeal:
- CMS-1500 Claim Form
- Remittance (ERA)
- Claim History
-
Add attachments to the appeal (e.g. visit note, letter of medical necessity, etc.)
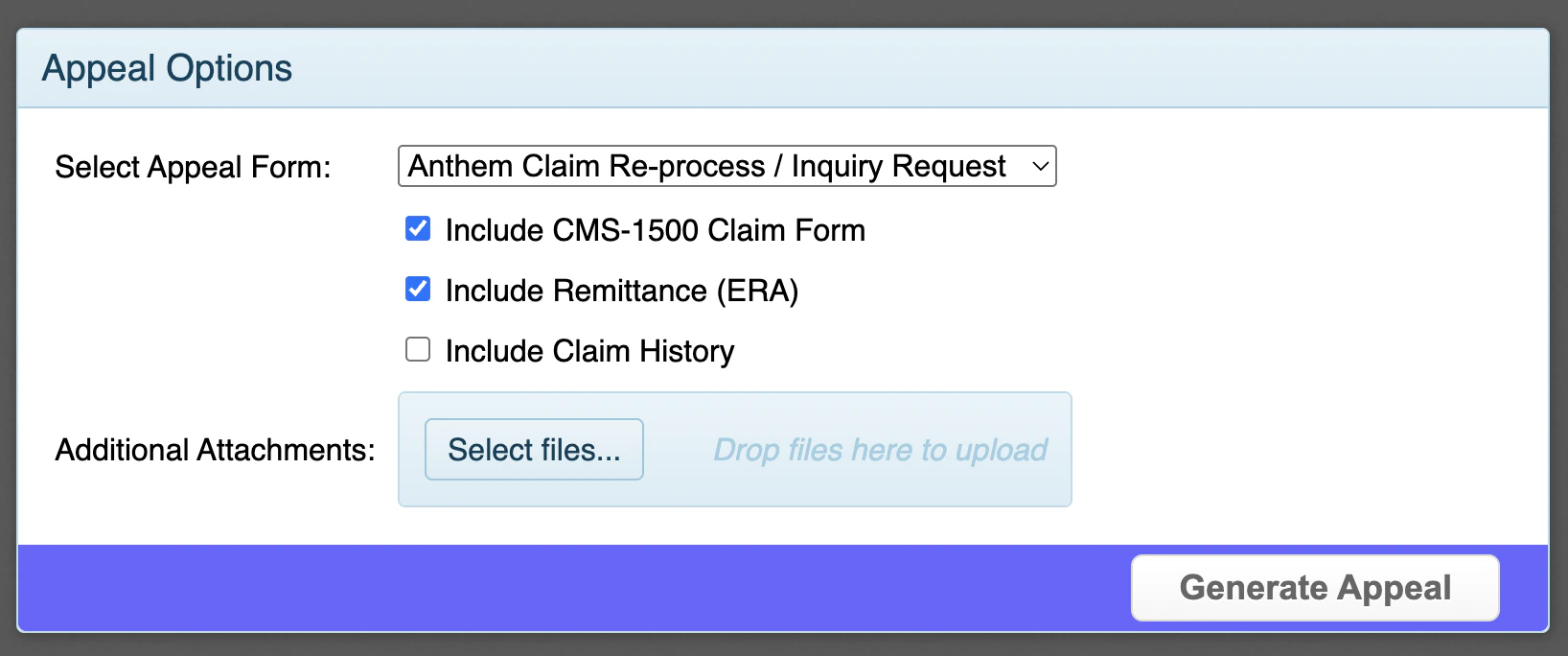
Choose your submission method:
- Electronic submission - Only available for some payers.
- Mailed by clearinghouse - Mailed on your behalf for an additional fee.
- Specify the mail to address and then click Send Mail.
- Faxed by clearinghouse - Faxed on your behalf for an additional fee.
- Specify a fax to number and then click Send Fax.
- Download and mail - Download the appeal packet at no additional cost and mail it yourself.
-
Click Manual Appeal and then download the the appeal packet.
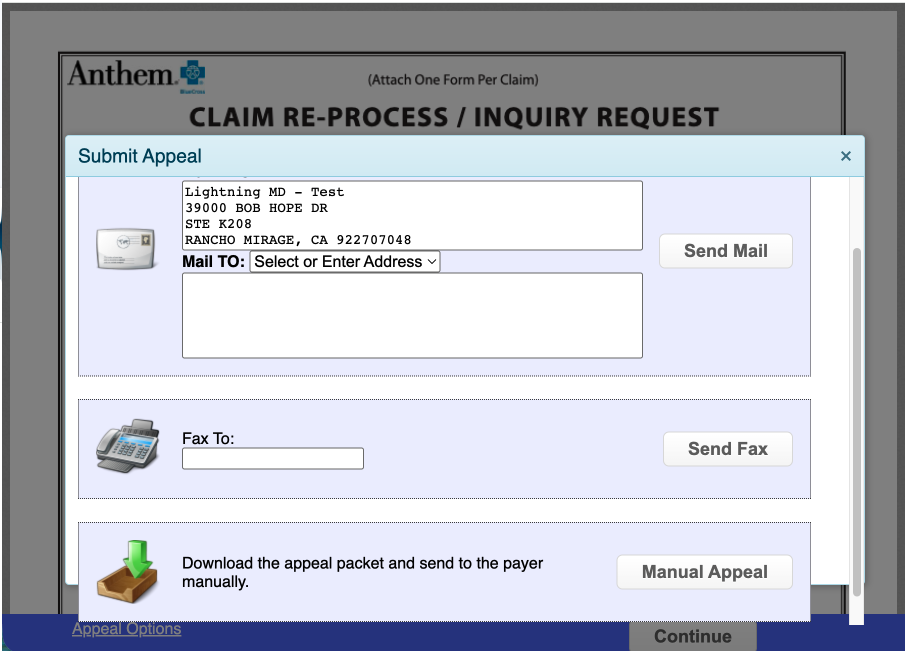
-
Click Manual Appeal and then download the the appeal packet.
For information on additional fees, see Fees Associated with Elation Billing.
Tracking the status of an appeal
Once an appeal has been generated, you can update the Tags on the claim to add the claim to an appeals Worklist for easier followup. See Using the Worklist for more information. For updates on the status of the appeal, contact the payer directly. You can use Claim Notes to track each follow-up.Acting on a claim after a decision is made on the appeal
- If the appeal is approved, the payer issues payment and a new ERA. You can post the payment to the claim like any other payment. The claim status updates accordingly in the Worklist.
- If the appeal is denied, review the payer’s response for the denial reason. Depending on the payer, you may be able to file a second-level appeal or escalate through the payer’s grievance process.
FAQ
Can I edit or resubmit an appeal after generating it?
Can I edit or resubmit an appeal after generating it?
Once an appeal is generated, you can start a new appeal on the same claim by repeating the steps above. Contact the payer directly if you need assistance with an appeal that was already submitted.
The Appeal button isn't showing up — what should I do?
The Appeal button isn't showing up — what should I do?
